A New Standard in Podiatric Surgery
From Blind Cuts to Precision Guidance
Minimally invasive foot surgery (MIS) has evolved dramatically since its 1960s origins, when surgeons relied on motorised burrs and blind osteotomies without internal fixation—a period marked by high complication rates. Today’s fourth-generation techniques combine purpose-built burrs, real-time fluoroscopy, and rigid screw fixation (e.g., the MICA procedure) to achieve reproducible, 3‑D‑guided corrections. This transformation has been driven by systematic reviews demonstrating that MIS reduces tissue trauma, lowers infection risk, and compresses recovery timelines, allowing patients to return to work or sport weeks earlier than with traditional open approaches.
A Philosophy, Not Just a Procedure
Leaders such as Dr. Amiethab Aiyer (Johns Hopkins) and the APMA 2025 round‑table panel—moderated by Kelsey Millonig, DPM, MPH—emphasise that MIS is a philosophy of patient‑centered care rather than a single technique. This mindset tailors the approach to each patient’s anatomy and lifestyle, applying small‑incision methods across bunions, hammertoes, Achilles pathology, and complex hindfoot fusions while preserving healthy tissue.
Advanced Foot Care IL: Embodying the Standard
At Advanced Foot Care IL’s NW Chicago and South‑Florida locations, this philosophy comes to life. Surgeons combine high‑tech MIS instrumentation with comprehensive pre‑operative education and personalised post‑operative support—including custom orthotics and regenerative adjuncts—to optimise healing and return patients to their daily lives with minimal downtime.
What’s Cutting‑Edge in the MIS Toolbox?
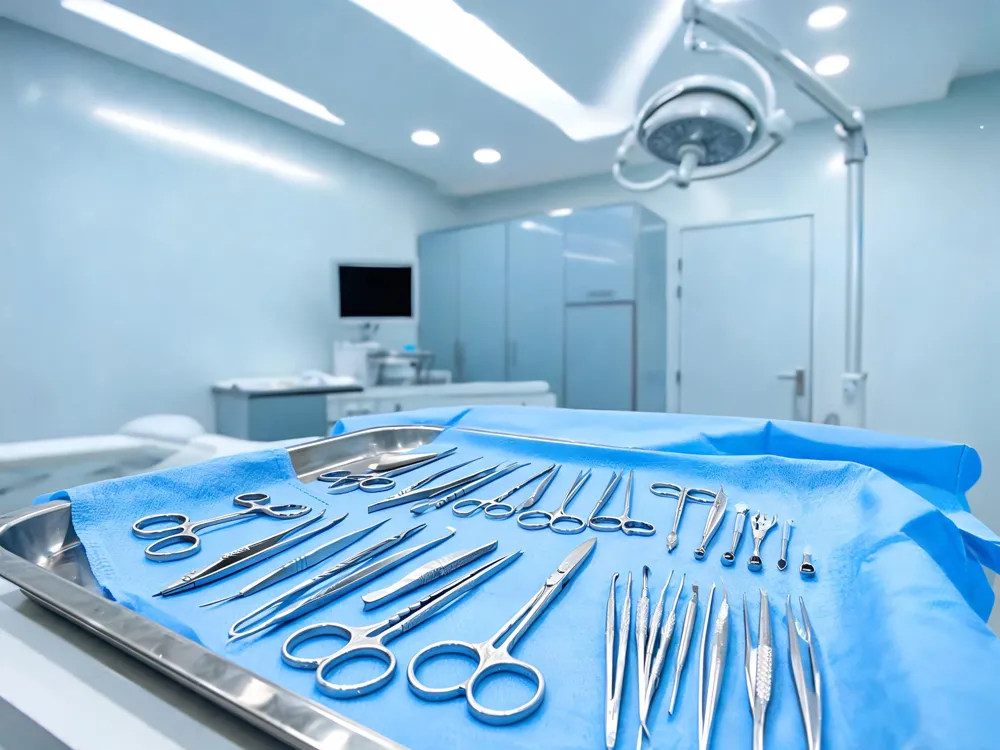
What’s Cutting‑Edge in the MIS Toolbox?
Modern MIS for hallux valgus has evolved to percutaneous Chevron‑Akin (MICA) and fourth‑generation transverse distal metatarsal osteotomies with dual‑screw fixation. These techniques achieve significantly better correction of the distal metatarsal articular angle (DMAA) and allow earlier weight‑bearing compared with open methods.
For lesser‑ray deformities, distal minimally invasive metatarsal osteotomies (DMMO) avoid shortening and dorsal displacement of the second and third metatarsals. This preserves forefoot biomechanics and delivers superior cosmetic outcomes, as supported by Neunteufel et al. (2022).
MIS for insertional Achilles tendinopathy uses small‑incision burr work with meticulous fluid irrigation to prevent thermal tissue injury. The approach yields complication rates roughly half those of open surgery, making it a strong option for younger, active patients with focal pathology.
Mini‑fusion techniques for subtalar, tibiotalocalcaneal (TTC), and ankle arthrodeses rely on windshield‑wiper burrs, arthroscopic scopes, and 3‑D navigation. These tools enable precise joint preparation while minimising wound‑healing problems, especially in high‑risk patients.
Robotic‑assisted platforms and computer‑guided navigation improve screw‑placement accuracy in complex reconstructions. They are complemented by low‑speed (<10,000 rpm) high‑torque burrs with integrated irrigation, 3‑D‑printed patient‑specific guides, and emerging virtual‑reality planning tools that together expand the precision and safety of the modern MIS toolbox.
Can a Podiatrist Repair an Achilles Tendon?
Yes, Foot and Ankle Surgeons Specialize in Achilles Repair
Podiatric surgeons, especially those with advanced foot and ankle training, are fully licensed to repair Achilles tendon ruptures and chronic insertional tendinopathy. Our team routinely performs these repairs using minimally invasive techniques that dramatically reduce tissue disruption.
The Minimally Invasive Approach
Modern Achilles repair typically begins with a 2–5 mm incision. The surgeon uses a percutaneous burr to debride the diseased insertion and then secures the tendon with small-profile sutures or screws. This results in an incision roughly half the length of traditional open surgery, preserving surrounding soft tissues.
Faster Recovery, Fewer Complications
Patients often bear weight immediately in a protective boot, resume normal activities sooner, and face significantly lower wound-healing complications. The 2025 APMA National Conference panel reported that for younger, active patients with focal insertional Achilles pathology, the minimally invasive approach halved complication rates compared with open surgery—though large calcaneal spurs may still require open exposure.
Our Clinic’s Comprehensive Protocol
We offer this procedure at both our NW Chicago and South Florida locations. The surgery is performed under regional nerve blocks with light sedation. Postoperatively, we follow a structured rehabilitation plan that includes early mobility, compression therapy, and optional low-level laser or PRP injections to accelerate healing and reduce inflammation.
Evidence‑Based Benefits and the Learning Curve

How do the outcomes of minimally invasive foot surgery compare to open techniques?
Minimally invasive surgery (MIS) offers measurable statistical advantages. Compared with traditional open procedures, MIS reduces wound‑infection rates by up to 50 %, substantially lowers intra‑operative blood loss, and shortens operative times. For bunion corrections, patients report needing an average of only two pain pills after surgery—a dramatic reduction in opioid reliance.
What recovery timeline can patients expect?
Many MIS patients bear weight immediately after surgery in a protective boot. Return to lightweight shoes typically occurs within 4–6 weeks, with full functional recovery in 6–12 weeks. For fracture‑related MIS, healing benchmarks are slightly longer: most patients resume walking within 6–8 weeks.
What is the learning curve for surgeons?
The MIS learning curve is steep. Studies by Baumann (2023) and Lewis (2023) show surgeons require 35–40 cases to reach proficiency in hallux valgus procedures. While operative and fluoroscopy times decrease, complication rates remain low throughout the learning process, provided surgeons adhere to structured training.
Why is mentorship critical?
Panelists at the 2025 APMA National conference emphasized that formal mentorship, cadaver labs, and repeated practice are essential. This is especially true for complex fusions and calcaneal osteotomies, where nuanced technique directly affects outcomes.
Are long‑term outcome gaps a concern?
Short‑term data for MIS are robust, but longitudinal studies remain limited for newer techniques such as percutaneous tarsometatarsal fusions. Ongoing research is needed to confirm durability and refine patient selection.
Putting the Patient First: Evaluation, Selection, and Holistic Recovery
Comprehensive Pre‑Operative Work‑Up
A thorough evaluation is essential. Surgeons use weight‑bearing X‑rays, CT/MRI for complex deformities, and gait analysis to plan the procedure. For diabetic or elderly patients, a vascular assessment minimizes wound‑healing risks.
Patient Selection Criteria
Ideal candidates have mild‑to‑moderate deformities, are in good overall health, desire a faster return to activity, and have not responded to conservative care. Contraindications include severe osteoporosis, massive calcaneal spurs, or extensive joint instability. Careful selection ensures optimal outcomes.
Insurance and Cost Considerations
Many insurers now cover MIS when deemed medically necessary. While upfront equipment costs can be higher, the total cost of care is often lower due to fewer complications and a quicker return to work. Some clinics offer direct‑pay models to bypass insurance restrictions.
Adjunctive Therapies for Optimal Healing
Post‑operative care includes compression socks to reduce swelling, low‑level laser therapy, PRP or amniotic injections, structured physical therapy, anti‑inflammatory diet, and mental‑wellness support. These therapies accelerate recovery and improve long‑term function.
Real‑World Success Stories
Clinics such as North Texas Podiatry Associates, Hall Podiatry, and Stride Forward Podiatry demonstrate that outpatient MIS can achieve same‑day discharge, minimal scarring, and rapid functional gains. These examples highlight how personalized, holistic care enhances patient satisfaction and outcomes.
The Future of Minimally Invasive Podiatry at Advanced Foot Care IL
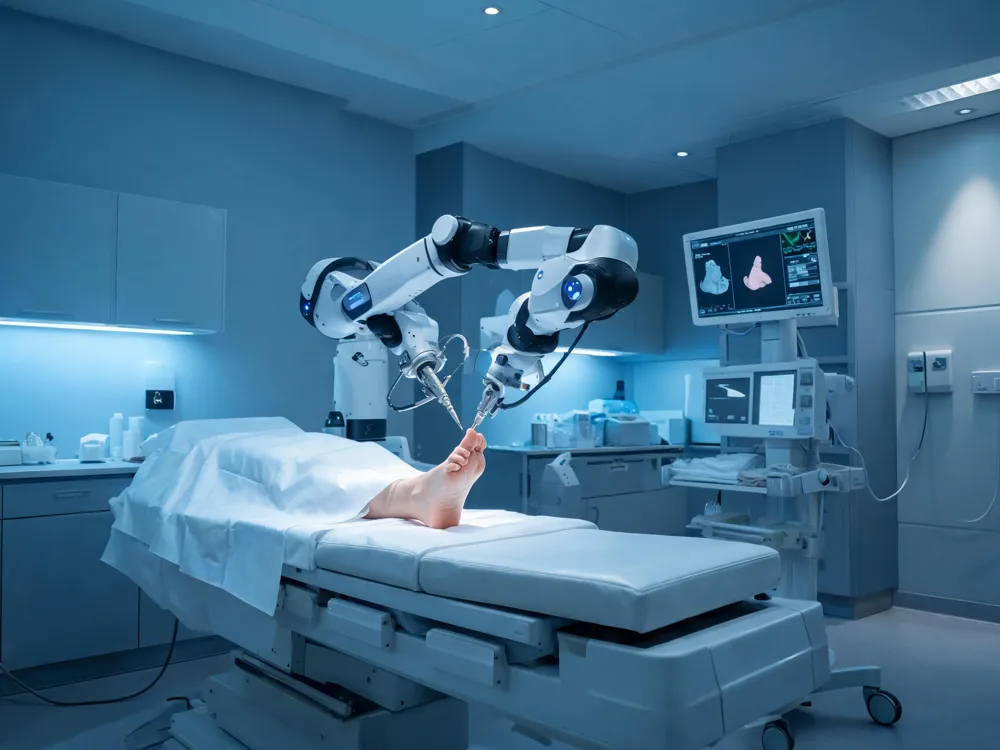
Emerging Innovations – Precision Without Compromise
Next-generation robotic arms and AI-driven intra-operative navigation are entering MIS practice, promising even smaller incisions and greater accuracy. Fully 3D-printed, patient-specific instruments will soon allow surgeons to tailor hardware and guides to each foot’s unique anatomy, reducing operating time and improving alignment.
Research Pipeline – Building Evidence
Ongoing comparative trials—such as those highlighted at the APMA round‑table—track hallux valgus recurrence and hardware‑removal rates in longitudinal registries. Biomechanical studies are now examining percutaneous flat‑foot reconstructions, evaluating how MIS osteotomies affect dynamic foot function and long‑term stability.
Commitment to Education – Mastery Through Mentorship
Advanced Foot Care IL offers a dedicated in‑house MIS fellowship, quarterly cadaver workshops, and tele‑mentoring with leaders such as Dr. Aiyer (Johns Hopkins) and Dr. Bernstein (Hudson Regional). This layered training ensures every surgeon reaches the competence plateau safely.
Community Outreach – Access for All
Free MIS consultation clinics and patient‑education webinars explain the what‑to‑expect timeline. Adopting the direct‑pay philosophy from Dr. Joel Foster’s Kansas City practice, we provide transparent pricing that makes advanced care accessible without insurance limitations.
Bottom Line
Bottom Line
Minimally invasive surgery (MIS) has evolved from a niche technique to the backbone of modern podiatric surgery, delivering superior cosmetic, functional, and economic outcomes across a wide range of foot and ankle pathologies. Our Northwest Chicago and South Florida clinics combine the latest technology with expert training, enabling podiatrists to safely perform Achilles tendon repairs, bunion corrections, hammertoe treatments, and complex fusions through incisions a fraction of the size of traditional approaches. Patients benefit from faster healing, less pain, and a quicker return to activities—from walking the dog to running a marathon or simply wearing a sandal.
