Welcome to Advanced Foot & Ankle Care
Onychomycosis, or nail fungus, is a common fungal infection that thickens, discolors, and makes nails brittle. Recent advances in podiatry have highlighted laser therapy as a minimally invasive option that targets fungal cells beneath the nail plate without systemic drug exposure. This article first outlines the clinical presentation and risk factors of nail fungus, then explains why lasers—particularly Nd:YAG and fractional CO₂ devices—are gaining attention for their modest cure rates (40‑70%) and low side‑effect profile, and finally describes the structure of the following sections, which cover treatment protocols, combination strategies, post‑procedure care, and cost considerations.
Understanding the Types and Causes of Nail Fungus
Types of Onychomycosis & Key Risk Factors
| Type | Typical Presentation | Common Pathogen | Main Risk Factors |
|---|---|---|---|
| Distal/Lateral Subungual | Yellowing, thickening, brittleness starting at nail tip | Dermatophytes (Trichophyton) | Warm, moist shoes; minor trauma; athlete’s foot |
| White Superficial | White, crumbly patches on nail surface | Dermatophytes (Trichophyton mentagrophytes) | Public showers, swimming pools, damp environments |
| Proximal Subungual | Starts near cuticle, spreads outward; often in immunocompromised | Dermatophytes (Trichophyton) | Immunosuppression, diabetes, vascular disease |
| Candida‑type | Redness, swelling around nail, often with skin involvement | Yeast (Candida) | Moist environments, frequent water exposure, compromised immunity |
| Mixed Bacterial‑Fungal | Severe discoloration, odor, pain | Bacteria + fungi | Poor foot hygiene, repeated trauma, chronic nail dystrophy |
Risk factors across all types: prolonged moisture, nail trauma, athlete’s foot, diabetes, peripheral vascular disease, immunosuppression, reuse of unclean nail‑care tools.
 Onychomycosis presents in several clinical forms. The most common is distal (or lateral) subungual onychomycosis, which begins at the nail tip and spreads inward, producing yellowing, thickening and brittleness. White superficial onychomycosis appears as white, crumbly patches on the surface of the nail plate. Proximal subungual onychomycosis starts near the cuticle and moves outward, often seen in immunocompromised patients. Candida‑type onychomycosis, caused by yeast rather than dermatophytes, may be accompanied by surrounding skin redness and swelling. Mixed bacterial‑fungal infections can also occur, leading to more severe discoloration, odor, and pain.
Onychomycosis presents in several clinical forms. The most common is distal (or lateral) subungual onychomycosis, which begins at the nail tip and spreads inward, producing yellowing, thickening and brittleness. White superficial onychomycosis appears as white, crumbly patches on the surface of the nail plate. Proximal subungual onychomycosis starts near the cuticle and moves outward, often seen in immunocompromised patients. Candida‑type onychomycosis, caused by yeast rather than dermatophytes, may be accompanied by surrounding skin redness and swelling. Mixed bacterial‑fungal infections can also occur, leading to more severe discoloration, odor, and pain.
Risk factors include prolonged exposure to warm, moist environments—such as sweaty shoes, gym locker rooms, public showers, and swimming pools—where dermatophytes, yeasts, and molds thrive. Minor nail trauma, cracks, or separation of the nail plate create portals for fungal entry. Individuals with athlete’s foot, diabetes, peripheral vascular disease, or compromised immunity are especially vulnerable. Reusing unclean nail‑care instruments can further spread the infection.
Diagnostically, a thorough history and physical examination are essential. Confirmation is usually achieved by potassium‑hydroxide preparation, fungal culture, or nail‑clipping microscopy to differentiate true infection from dystrophy or psoriasis. Early identification guides appropriate therapy, whether topical, oral, or laser‑based.
Laser Treatment Mechanics, Options, and Clinical Evidence
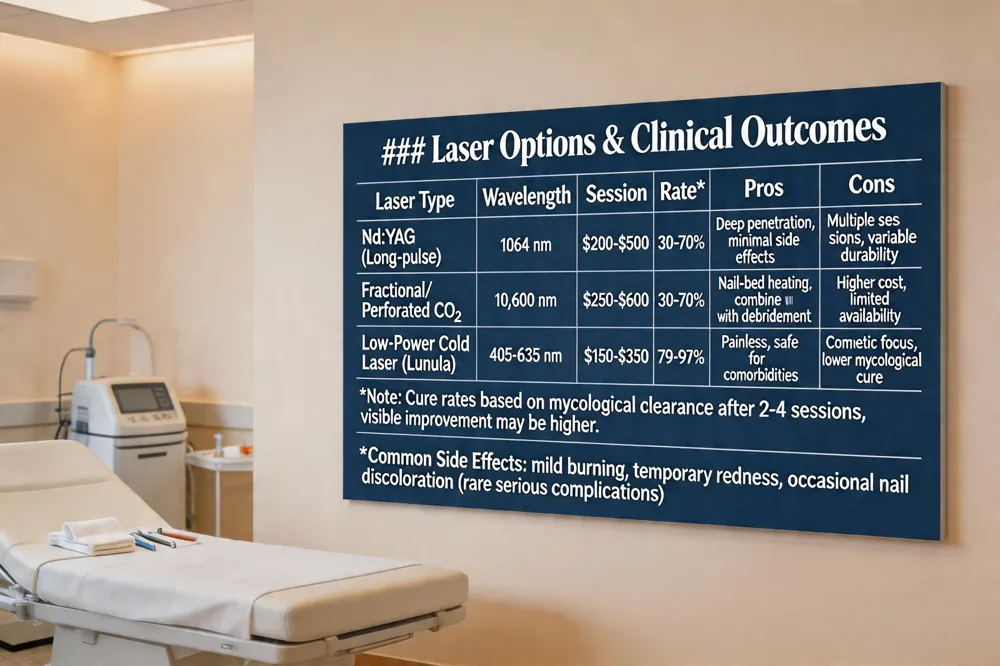
Laser Options & Clinical Outcomes
| Laser Type | Wavelength | Typical Session Cost | Reported Mycological Cure Rate* | Pros | Cons |
|---|---|---|---|---|---|
| Nd:YAG (Long‑pulse) | 1064 nm | $200‑$500 | 30‑70 % (up to 71 % in meta‑analysis) | Deep penetration, minimal systemic side effects | Requires multiple sessions, variable durability |
| Fractional/Perforated CO₂ | 10,600 nm | $250‑$600 | 30‑70 % (up to 95 % for perforated) | Excellent nail‑bed heating, can be combined with debridement | Higher cost, limited availability |
| Low‑Power Cold Laser (e.g., Lunula) | 405‑635 nm | $150‑$350 | 79‑97 % clearance (cosmetic) | Painless, safe for comorbidities | Primarily cosmetic, lower mycological cure |
Note: Cure rates are based on mycological clearance after 2‑4 sessions; clinical (visible) improvement may be higher.
Common Side Effects: mild burning, temporary redness, occasional nail discoloration (rare serious complications).
 Laser therapy for onychomycosis works by delivering specific wavelengths that penetrate the nail plate and heat fungal cells to 40‑60 °C, disrupting their DNA and metabolism while sparing surrounding tissue. The most common devices are Nd:YAG (1064 nm) lasers, fractional or perforated CO₂ lasers; each is selected for its ability to reach the nail bed and be absorbed by fungal chromophores.
Laser therapy for onychomycosis works by delivering specific wavelengths that penetrate the nail plate and heat fungal cells to 40‑60 °C, disrupting their DNA and metabolism while sparing surrounding tissue. The most common devices are Nd:YAG (1064 nm) lasers, fractional or perforated CO₂ lasers; each is selected for its ability to reach the nail bed and be absorbed by fungal chromophores.
Clinical studies report mycological cure rates ranging from 30‑70 % after 2‑4 sessions, with some meta‑analyses showing up to 71 % for long‑pulse Nd:YAG and 95 % for perforated CO₂. Combined with topical or oral antifungals, outcomes improve further. Benefits include minimal invasiveness, lack of systemic side effects, and rapid office visits. Drawbacks are the need for multiple sessions, variable long‑term durability, and out of‑pocket costs ($200–$500 per session, often cosmetic‑only coverage).
Pros and cons of laser treatment for toenail fungus – Precise, painless, no liver toxicity; however, multiple visits are required, costs can be high, and cure durability is not fully proven.
Best laser treatment for nail fungus – Low‑power, cold‑laser systems (e.g., Lunula Cold Laser) achieve 79‑97 % clearance with minimal discomfort, making them suitable for patients with comorbidities.
What kills toenail fungus instantly – No instant cure; oral antifungals or professional laser therapy are the fastest, yet both need weeks‑to‑months for nail regrowth.
What kills toenail fungus permanently – A full course of oral terbinafine or itraconazole (12 weeks) or combined laser‑plus‑topical regimens, followed by diligent foot hygiene.
Side effects of laser toenail fungus treatment – Mild burning, temporary redness, occasional nail discoloration; serious complications are rare.
Two drawbacks of laser therapy – Requires several sessions, increasing cost and treatment time; results can vary widely based on nail thickness, laser type, and patient factors.
Choosing the Right Treatment Path: Oral, Topical, and Combination Strategies
Treatment Modalities Comparison
| Modality | Typical Agents | Course Duration | Reported Cure Rate (clinical) | When to Use |
|---|---|---|---|---|
| Oral Antifungals | Terbinafine, Itraconazole | 6‑12 weeks (Terbinafine) / 12 weeks (Itraconazole pulse) | 70‑90 % (Terbinafine) | Moderate‑to‑severe disease, patients without liver issues |
| Topical Lacquers | Ciclopirox, Efinaconazole, Tavaborole | 48‑52 weeks (daily) | 10‑30 % | Early‑stage disease, contraindication to oral meds, adjunct after debridement |
| Combination (Oral + Laser + Topical) | Any oral + Nd:YAG/CO₂ + topical | 6‑12 weeks oral + 2‑4 laser sessions | 70‑90 % (oral) + 30‑70 % (laser) → higher durability, relapse <20 % | Patients seeking maximal cure, those with thick nails or mixed infections |
| Laser + Debridement + Topical | Nd:YAG/CO₂ + nail debridement + topical | 2‑4 laser sessions + ongoing topical | 30‑70 % (laser alone) → improved when combined | Patients unable to take oral meds, early‑stage disease, cosmetic improvement |
Key Takeaway: Oral terbinafine remains the most effective single therapy; lasers serve as valuable adjuncts, especially when oral therapy is contraindicated.
 Onychomycosis can be tackled with oral drugs, topical agents, or a blend of methods.
Onychomycosis can be tackled with oral drugs, topical agents, or a blend of methods.
Standard oral antifungal options and success rates – Prescription oral terbinafine (Lamisil) remains the highest‑rated therapy, delivering 70‑90 % cure rates for moderate‑to‑severe infections with a typical 6‑12‑week course. Itraconazole is an alternative, especially for patients with mixed‑species infections, but both require liver‑function monitoring.
Topical nail lacquers and when they are appropriate – Topicals such as ciclopirox, efinaconazole, and tavaborole penetrate the nail plate poorly, yielding 10‑30 % cure rates. They are best reserved for early‑stage disease, patients who cannot take oral medication, or as adjuncts after debridement.
Combination approaches with laser and debridement – Nd:YAG (1064 nm) or fractional CO₂ lasers heat the nail bed, achieving 30‑70 % mycological cure after 2‑4 sessions. When paired with nail debridement and topical antifungals, success improves and relapse drops to <20 % in one year.
Clinic‑specific advanced medical footcare services – Centers such as Oklahoma Foot & Ankle Associates, Advanced Podiatry, and Diablo Foot & Ankle provide integrated laser therapy, professional debridement, and personalized foot‑hygiene counseling, ensuring optimal outcomes for each patient.
Key takeaways – Oral terbinafine is the most effective single modality; lasers are valuable adjuncts for patients who cannot tolerate systemic drugs; and a multimodal plan—combining oral or topical agents with laser and meticulous after‑care—offers the highest likelihood of durable cure.
Practical Considerations: Cost, Insurance, and Access to Care
Cost, Insurance & Accessibility Snapshot
| Item | Typical Price Range | Total Cost (2‑4 Sessions) | Insurance Coverage | Common Locations |
|---|---|---|---|---|
| Nd:YAG Laser Session | $200‑$400 | $500‑$1,200 | Generally not covered (cosmetic classification) | Oklahoma Foot & Ankle Associates (OK), Advanced Foot & Ankle Center (IL/FL), regional podiatry clinics |
| Fractional CO₂ Laser Session | $250‑$600 | $600‑$1,400 | Not covered | Same as above, plus select dermatology offices |
| Low‑Power Cold Laser (Lunula) | $150‑$350 | $300‑$1,050 | Not covered | Specialty foot‑care clinics, some retail health centers |
| Oral Antifungal (Terbinafine 12‑week) | $30‑$80 (generic) | $30‑$80 | Frequently covered (prescription drug benefit) | Pharmacies, tele‑medicine providers |
| Topical Lacquer (Efinaconazole) | $200‑$250 per 12‑week bottle | $200‑$250 | May be partially covered (depends on plan) | Pharmacies, dermatology clinics |
Financing Options: HSAs/FSAs, clinic‑provided payment plans, package discounts (e.g., complimentary third session for multi‑nail treatment).
 Typical price ranges for laser series
Typical price ranges for laser series
Laser therapy for onychomycosis is usually billed per session, with costs ranging from $200‑$400. A typical treatment course consists of 2‑4 sessions, bringing the total out between $500 and $1,200. Prices vary with the number of nails treated, the severity of the infection, and the laser system used (e.g., Nd:YAG, CO₂, PinPointe™). Some clinics offer package discounts or a complimentary third session for multi‑nail cases.
Insurance coverage status
Because laser nail treatment is classified as a cosmetic procedure, most private insurers and Medicare consider it experimental and do not reimburse the cost. Patients often rely on out‑of‑pocket payment, health‑savings accounts (HSAs), flexible‑spending accounts (FSAs), or clinic‑provided financing plans.
Clinic locations and scheduling
Several reputable podiatry practices provide laser therapy: Oklahoma Foot and Ankle Associates (Edmond, Moore, Midwest City, OK), Advanced Foot & Ankle Center (northwest Chicago and South Florida), and many regional foot clinics across the United States. To schedule, contact the office directly or use the provider’s online booking portal; most clinics require a pre‑treatment evaluation to confirm eligibility.
Mayo Clinic perspective
The Mayo Clinic acknowledges laser therapy as an adjunctive option but notes limited high‑quality evidence for cure. It generally recommends oral antifungals or medicated nail polish as first‑line treatments. When laser is chosen, Mayo advises patients that multiple sessions are often needed, outcomes can be variable, and the procedure is typically not covered by insurance.
Patient Guidance, Aftercare, and Long‑Term Success
After‑Care Checklist & Signs of Recovery
| After‑Care Action | Frequency | Purpose |
|---|---|---|
| Keep feet dry & breathable | Daily | Reduces fungal growth environment |
| Trim and file nails straight | 2‑3 times/week | Improves laser penetration, reduces trauma |
| Wear moisture‑wicking socks & breathable shoes | Daily | Maintains dry environment |
| Schedule follow‑up nail check (every 3–6 months) | Quarterly | Detect early recurrence |
How to Know the Fungus Is Dying:
- New nail growth starts at the cuticle, appears smoother, pinker, and less thick.
- Discoloration stops advancing upward.
- Nail becomes easier to trim and less brittle.
Relapse Prevention:
- Continue foot hygiene for at least 6 months after cure.
- Avoid sharing nail tools; disinfect regularly.
- Re‑treat any new lesions promptly.
Home Laser Devices: Cosmetic‑only FDA‑cleared; provide modest cosmetic improvement but lack the energy needed for true mycological cure. Professional office‑based lasers remain the recommended option for durable results.
 Laser treatment for toenail fungus reviews – Clinical studies report mixed outcomes: cure rates range 30‑70 % after 2‑4 sessions, with many patients noting rapid nail‑clarity improvement and minimal discomfort. Effectiveness is higher when a podiatrist combines laser with topical or oral antifungals, especially for early‑stage or moderate disease. Does fungus come back after laser treatment? – Recurrence is common if spores remain or foot hygiene lapses. Maintaining dry, breathable footwear, using antifungal powders, and regular follow‑up visits reduce relapse, which can reach up to 20 % within a year. How to know if toenail fungus is dying – New, healthier nail begins at the cuticle, appearing smoother, pinker, and less thick. Discoloration stops spreading upward, and the nail becomes easier to trim. Changes appear over weeks to months due to slow nail growth. Toenail fungus laser treatment at home – Over‑the‑counter laser/LED devices are FDA‑cleared for cosmetic use only; they often lack the energy to penetrate thick nails and show modest, temporary improvement. They are not a reliable substitute for office‑based therapy, especially in severe or multi‑nail cases. Do home nail fungus lasers work – Evidence is weak; they may lighten mild infections but rarely achieve lasting eradication. Professional in‑office lasers, delivering controlled 1064 nm energy, yield higher mycological cure rates and are recommended for most patients. Laser treatment for nail fungus at home – Home devices can aid cosmetic appearance but do not guarantee cure or prevent recurrence. For thick, dystrophic nails or patients with diabetes, a podiatrist‑supervised laser protocol combined with proper foot care remains the most effective strategy.
Laser treatment for toenail fungus reviews – Clinical studies report mixed outcomes: cure rates range 30‑70 % after 2‑4 sessions, with many patients noting rapid nail‑clarity improvement and minimal discomfort. Effectiveness is higher when a podiatrist combines laser with topical or oral antifungals, especially for early‑stage or moderate disease. Does fungus come back after laser treatment? – Recurrence is common if spores remain or foot hygiene lapses. Maintaining dry, breathable footwear, using antifungal powders, and regular follow‑up visits reduce relapse, which can reach up to 20 % within a year. How to know if toenail fungus is dying – New, healthier nail begins at the cuticle, appearing smoother, pinker, and less thick. Discoloration stops spreading upward, and the nail becomes easier to trim. Changes appear over weeks to months due to slow nail growth. Toenail fungus laser treatment at home – Over‑the‑counter laser/LED devices are FDA‑cleared for cosmetic use only; they often lack the energy to penetrate thick nails and show modest, temporary improvement. They are not a reliable substitute for office‑based therapy, especially in severe or multi‑nail cases. Do home nail fungus lasers work – Evidence is weak; they may lighten mild infections but rarely achieve lasting eradication. Professional in‑office lasers, delivering controlled 1064 nm energy, yield higher mycological cure rates and are recommended for most patients. Laser treatment for nail fungus at home – Home devices can aid cosmetic appearance but do not guarantee cure or prevent recurrence. For thick, dystrophic nails or patients with diabetes, a podiatrist‑supervised laser protocol combined with proper foot care remains the most effective strategy.
Putting It All Together – Your Path to Healthy Nails
Treating onychomycosis begins with a thorough podiatric evaluation to confirm the fungus and assess nail thickness, vascular health, and comorbidities. Options range from evidence‑based oral antifungals (terbinafine, itraconazole) with 55‑70% cure rates, to topical lacquers that penetrate poorly, to emerging laser therapies that use Nd:YAG or CO₂ wavelengths to heat the nail bed without systemic side effects. Laser protocols typically involve 2‑4 sessions spaced weeks apart, often combined with debridement or adjunctive antifungals to boost success. After treatment, patients should maintain foot hygiene, wear breathable shoes, and schedule follow‑up visits to monitor regrowth and prevent recurrence.
