Understanding Ingrown Toenails
What Is an Ingrown Toenail?
An ingrown toenail occurs when the side or corner of a toenail penetrates the surrounding skin, most often on the big toe. This triggers inflammation, pain, redness, and swelling. If the skin barrier is broken, bacteria can enter, leading to infection with symptoms such as throbbing pain, pus, warmth, and even fever.
Primary Causes and Risk Factors
| Cause | Description | Why It Matters |
|---|---|---|
| Improper nail trimming | Cutting nails too short or rounding the edges | Creates a sharp spike that can embed into the skin |
| Tight or narrow footwear | Shoes that compress the toes, especially high heels | Forces the nail edge into the surrounding tissue |
| Genetic nail shape | Naturally curved, fan-shaped, or thick nails | Increases predisposition to ingrowth |
| Toe trauma | Stubbing or dropping an object on the toe | Alters nail growth direction |
| Foot deformities | Bunions, hammertoes, or excessive pronation | Changes mechanical pressure on the nail bed |
People with diabetes, peripheral neuropathy, or poor circulation face higher risks of severe complications because reduced sensation masks early infection and impaired healing worsens outcomes.
Why Professional Care Matters
Attempting "bathroom surgery" with household tools like nail clippers, tweezers, or needles often damages the nail matrix, introduces bacteria, and leaves spicules behind. This can turn a simple irritation into a deeper infection requiring antibiotics or hospitalization. A podiatrist uses sterile instruments and local anesthesia to precisely remove the offending nail edge, providing immediate relief and a path to proper healing. For recurrent cases, minimally invasive matrix ablation can permanently prevent the problematic corner from growing back, lowering recurrence to under 5%
Common DIY Mistakes That Worsen the Problem
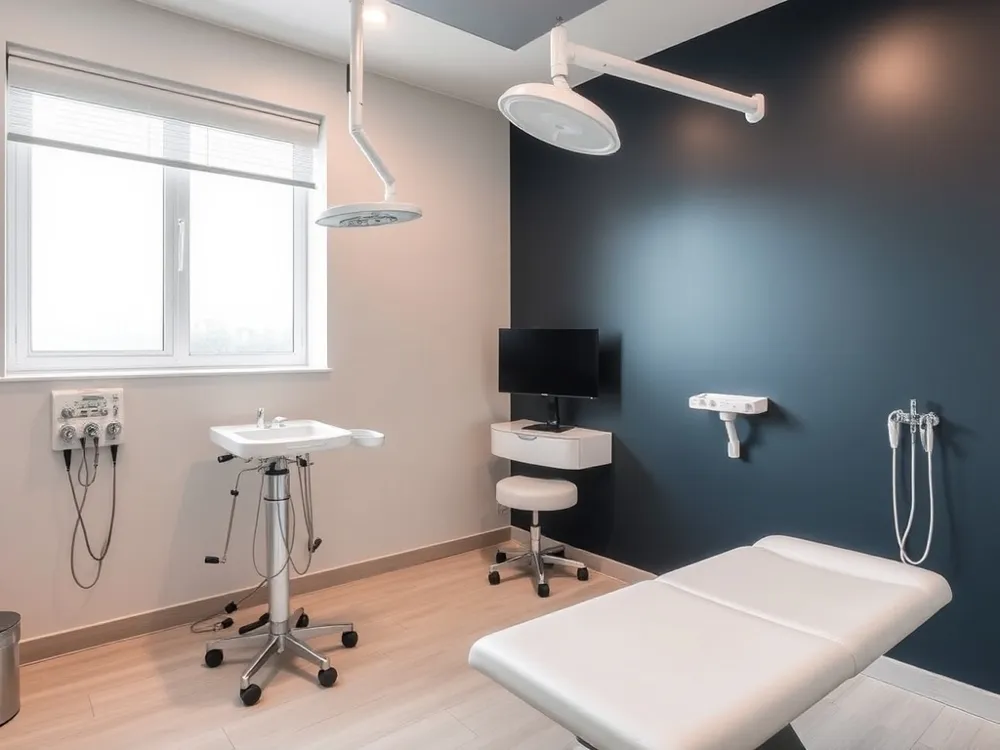
How to remove an ingrown toenail yourself—and why most methods fail
Many people search for a quick way to remove an ingrown toenail at home. The safest approach for a mild case involves soaking the foot in warm, soapy water for 15–20 minutes several times daily, then gently lifting the nail edge with a clean piece of waxed dental floss or cotton. Apply an over-the-counter antibiotic ointment and wear roomy shoes. However, attempting to cut or tear the nail yourself with non-sterile tools such as nail clippers, tweezers, or knives dramatically increases infection risk. These tools introduce bacteria into inflamed tissue, often causing cellulitis or abscess formation. Professional removal by a podiatrist under local anesthesia is the only safe method for significant or painful ingrown nails.
What makes an ingrown toenail worse? Common at-home errors
Four frequent mistakes turn a manageable ingrown toenail into a serious problem:
| Mistake | Why It Worsens the Condition | Safer Alternative |
|---|---|---|
| Cutting the nail too short or rounding edges | Prompts the sharp nail corner to grow into the skin, deepening the wound | Trim straight across, leaving a small white edge at the tip |
| Digging out the ingrown portion with sharp objects | Damages the nail matrix and leaves spicules behind, leading to abnormal regrowth and infection | Let a podiatrist perform a partial nail avulsion under sterile conditions |
| Applying cotton or floss incorrectly | Packs material too tightly, trapping moisture and bacteria against the skin, increasing infection | Use a thin, clean piece of waxed floss, replace it daily after soaking |
| Using non-sterile tools (clippers, scissors, knives) | Introduces pathogens into open wounds, risking cellulitis, osteomyelitis, or systemic infection | Use only sterilized instruments or seek professional care |
Ingrown toenail at base of nail—why professional care matters
An ingrown toenail at the base of the nail near the root causes intense pain, swelling, and often infection. This is especially dangerous for people with diabetes, peripheral neuropathy, or poor circulation, as healing is delayed and infection can spread rapidly. Home attempts to cut or lift the nail in this area can damage the nail matrix permanently. A podiatrist can safely perform a partial nail avulsion with or without matrix ablation to prevent recurrence and preserve healthy nail growth. If you notice pus, spreading redness, or fever, seek medical attention immediately.
When Home Care Isn’t Enough: Infection Signs & Diabetes Risks
 Properly identifying when an ingrown toenail has moved beyond a manageable nuisance is critical. While early-stage discomfort may respond to warm soaks and careful trimming, advancing symptoms demand professional evaluation. The distinction between simple inflammation and a spreading infection is the first line of defense in preventing serious complications.
Properly identifying when an ingrown toenail has moved beyond a manageable nuisance is critical. While early-stage discomfort may respond to warm soaks and careful trimming, advancing symptoms demand professional evaluation. The distinction between simple inflammation and a spreading infection is the first line of defense in preventing serious complications.
Can Diabetes Affect Ingrown Toenails?
Yes, diabetes significantly increases the risks associated with ingrown toenails. High blood glucose impairs circulation and the body's ability to fight infection. For someone with diabetes, a tiny break in the skin can rapidly become an ulcer. Peripheral neuropathy, common in diabetes, often masks the pain of an ingrown nail, allowing an infection to worsen unnoticed. This combination of poor blood flow and reduced sensation turns a minor nail issue into a potential threat. Because of the risk of gangrene and amputation, anyone with diabetes must seek podiatric care at the very first sign of an ingrown toenail rather than attempting home remedies.
Ingrown Toenail Infection: What to Watch For
The classic signs of an infected ingrown toenail include persistent redness and swelling that extends beyond the nail margin, throbbing pain, and purulent drainage or pus. The area may feel warm to the touch, and in more advanced cases, a foul odor may develop. If you notice red streaks moving up the foot or leg, or if you develop a fever or chills, the infection is likely systemic. These symptoms indicate that bacteria have breached the skin barrier, and home care is no longer sufficient. Professional treatment, which may include partial nail removal and antibiotics, is required to prevent the infection from spreading to the bone.
Can an Ingrown Toenail Kill You?
While extremely rare, an untreated infected ingrown toenail can be life-threatening. The primary danger is the infection spreading through the bloodstream, causing sepsis—a severe systemic response that can be fatal. This risk is almost exclusively seen in individuals with compromised immune systems, diabetes, or severe peripheral vascular disease. In these populations, what begins as a local infection can become a bone infection (osteomyelitis) or require amputation. For otherwise healthy people, ingrown nails are painful but not lethal. However, the rare potential for serious complications underscores the importance of seeking prompt care when infection signs appear. There is no scenario where prolonged self-treatment of an infected ingrown nail is safe.
| Symptom | Home Care Limit | When to See a Podiatrist |
|---|---|---|
| Mild redness & tenderness | Warm soaks, cotton lift | Not improving in 2–3 days |
| Redness spreading | Not safe | Immediate evaluation |
| Pus or cloudy drainage | Not safe | Requires drainage & antibiotics |
| Fever, chills, red streaks | Not safe | Emergency medical care |
| Diabetes or poor circulation | Not safe | At the first sign of any ingrown nail |
Professional Solutions: Permanent Fixes & Surgical Options
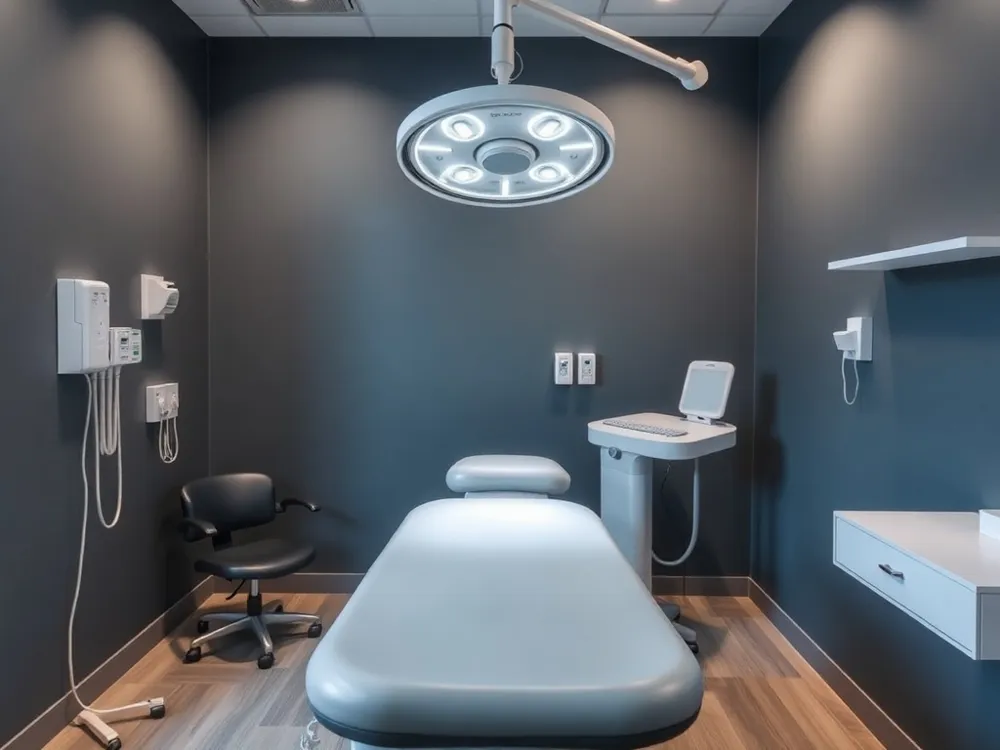 When home care fails or an ingrown toenail keeps coming back, a podiatrist can provide a permanent fix. The most effective procedure is a partial nail avulsion with chemical ablation. After numbing the toe with a local anesthetic, the podiatrist carefully removes the ingrown portion of the nail. Then, a small amount of a chemical, usually phenol, is applied to the nail matrix (the tissue where the nail grows). This prevents that specific section of the nail from growing back, reducing the recurrence rate from around 65% to under 10%.
When home care fails or an ingrown toenail keeps coming back, a podiatrist can provide a permanent fix. The most effective procedure is a partial nail avulsion with chemical ablation. After numbing the toe with a local anesthetic, the podiatrist carefully removes the ingrown portion of the nail. Then, a small amount of a chemical, usually phenol, is applied to the nail matrix (the tissue where the nail grows). This prevents that specific section of the nail from growing back, reducing the recurrence rate from around 65% to under 10%.
What does ingrown toenail surgery involve?
This minor, in-office procedure takes about 10 to 20 minutes. Other professional options include matrixectomy using a laser or electrocautery, which also destroys the nail matrix to prevent regrowth. These treatments are far more effective than home methods for resolving pain, infection, and inflammation caused by the nail digging into the skin.
What is recovery and aftercare like?
Recovery is generally quick and straightforward. Most patients can return to normal activities the very next day. You should keep the toe clean and dry, apply a prescribed topical antibiotic if needed, and wear open‑toed shoes or sandals for a few weeks. Avoid running, swimming, or soaking the foot for two weeks to protect the healing site. Over‑the‑counter pain relievers can manage any minor discomfort, and following these guidelines ensures a smooth recovery with a greatly reduced chance of the problem returning.
| Treatment | Procedure | Recurrence Rate | Recovery Time |
|---|---|---|---|
| Partial Nail Avulsion | Numb toe, remove ingrown edge | < 10% | Return next day |
| Chemical Matrixectomy | Apply phenol to nail matrix | < 10% | 1-2 weeks off activity |
| Laser Treatment | Laser ablation of nail matrix | Low (similar to chemical) | 1-2 days |
Footwear & Prevention: Choosing Shoes That Help, Not Harm
 A wide toe box is the cornerstone of ingrown‑nail‑friendly footwear. Shoes that allow the toes to lie flat without cramping keep pressure off the nail edges and reduce the chance of the nail digging into the skin. Look for models labeled "wide" (2E or wider) and avoid pointed or narrow toe shapes. Materials that wick moisture—such as breathable mesh, leather, or moisture‑wicking synthetics—keep the foot dry and discourage bacterial growth, which can turn a mild inflammation into infection.
A wide toe box is the cornerstone of ingrown‑nail‑friendly footwear. Shoes that allow the toes to lie flat without cramping keep pressure off the nail edges and reduce the chance of the nail digging into the skin. Look for models labeled "wide" (2E or wider) and avoid pointed or narrow toe shapes. Materials that wick moisture—such as breathable mesh, leather, or moisture‑wicking synthetics—keep the foot dry and discourage bacterial growth, which can turn a mild inflammation into infection.
Best shoes for ingrown toenails (women) – Choose styles with a rounded, spacious toe box, soft flexible uppers, and a half neither tight fit. Open‑toed sandals or slip‑ons eliminate contact with the affected nail, providing immediate relief while the toe heals.
New Balance options – The brand’s generous toe boxes and wide‑width range make it a podiatrist favorite. Popular choices include the 608 V5 cross‑trainer, 1122, 992, and 811 models, all praised for stability, cushioning, and minimal internal seams that reduce friction.
Prevention tip – Trim nails straight across, leave a small white edge, and keep feet clean and dry. For diabetics or those with poor circulation, extra vigilance and prompt podiatric evaluation are essential to avoid complications.
Safe At‑Home Symptom Management: Pain Relief, Soaks, and Medications

How to get rid of an ingrown toenail overnight
Completely resolving an ingrown toenail overnight is unlikely, but you can take steps for immediate relief. Soak your foot in warm water with Epsom salt for 15–20 minutes to soften the skin and nail. If there is no sign of infection, carefully place a small piece of sterile cotton or waxed dental floss under the ingrown edge to lift it away from the skin. Apply an over‑the‑counter antibiotic cream and wear open‑toed or loose‑fitting shoes to minimize pressure. For severe pain, discharge, or persistent issues, see a podiatrist.
Warm water and Epsom salt soaks
Warm water soaks are a first‑line, evidence‑based home treatment for mild ingrown toenails. Soak the affected foot in warm, soapy water or water with unscented Epsom salt for 10–20 minutes, three to four times daily. This routine reduces swelling, softens the nail and surrounding skin, and helps relieve tenderness. Do not use excessively hot water, as it can damage tissue and increase inflammation. After each soak, dry the foot thoroughly to prevent bacterial growth.
Proper use of cotton, floss, and antibiotic ointments
After soaking, gently lift the ingrown nail edge using a small piece of clean cotton or waxed dental floss. Place the material under the corner of the nail to encourage it to grow above the skin edge. Replace the cotton or floss daily, ideally after a shower when the skin is softer, and continue for about a week. Applying an over‑the‑counter antibiotic ointment (such as bacitracin, neomycin, or polymyxin) after cleaning helps prevent secondary bacterial infection. Cover the area with a clean bandage to protect it, but avoid using non‑sterile tools like nail clippers or knives to dig into the skin.
When to stop self‑care and seek a podiatrist
Home care is appropriate only for mild cases without signs of infection. Stop self‑treatment and see a podiatrist if you notice any of the following: severe throbbing pain, redness spreading up the toe, pus or cloudy drainage, foul odor, warmth around the nail, or fever. Individuals with diabetes, peripheral neuropathy, poor circulation, or weakened immune systems should seek professional evaluation immediately, as complications can progress rapidly. Also consult a podiatrist if symptoms do not improve after a few days of proper home care or if ingrown toenails recur frequently. Professional treatment options include partial nail avulsion or matrixectomy, which provide definitive relief and prevent recurrence.
Ingrown toenail treatment at home
For most mild ingrown toenails, start with at‑home care: soak the foot in warm, soapy water for 10–20 minutes, three to four times daily. After each soak, place a small piece of clean cotton or waxed dental floss under the ingrown edge to help the nail grow above the skin. Applying an over‑the‑counter antibiotic ointment and covering with a bandage can prevent infection. Avoid "bathroom surgery" with sharp tools. If you have diabetes, poor circulation, or signs of infection, see a podiatrist.
How to cut ingrown toenail at home
To cut an ingrown toenail at home, first soak the foot in warm, soapy water for 10–20 minutes to soften the nail. Gently lift the ingrown edge and place a small piece of wet cotton or waxed dental floss underneath. Trim the nail straight across, leaving 1–2 mm of white at the end, and avoid rounding the corners or cutting too short. Do not use manicure scissors to dig under the nail. If you notice redness, swelling, pus, or have diabetes, see a podiatrist instead.
Best antibiotic cream for ingrown toenail
For mild infections, topical antibiotic ointments such as polymyxin/neomycin (Neosporin) or mupirocin are commonly recommended. Apply after soaking the foot to help combat superficial bacteria and reduce inflammation. However, these creams treat symptoms, not the underlying nail problem. For persistent pain, discharge, or recurrent issues, professional evaluation is necessary to prevent complications and achieve long‑term relief.
How to drain pus from ingrown toenail
Do not attempt to drain pus from an ingrown toenail yourself using a needle or sharp object. Instead, soak the toe in warm water with unscented Epsom salts for 15 minutes several times a day to help draw out pus naturally and reduce swelling. After soaking, gently dry the area and apply an over‑the‑counter antibiotic ointment, covering it with a clean bandage. If pus persists, pain increases, or you have conditions like diabetes, see a podiatrist promptly for professional drainage and possible oral antibiotics. Professional care prevents the infection from spreading and ensures proper treatment.
| Home‑Care Method | How to Do It Safely | When to Stop & See a Podiatrist |
|---|---|---|
| Warm water + Epsom salt soaks | 10–20 min, 3–4 times daily | If swelling, pain, or redness increases |
| Placing cotton or dental floss | After soaking, gently lift nail edge | If area becomes more tender or bleeds |
| Topical antibiotic ointment | Apply after cleaning; cover with bandage | If pus, fever, or spreading redness appears |
| Trimming nail straight across | After softening, leave 1–2 mm white tip | If you have diabetes, neuropathy, or poor circulation |
Take the Right Steps Toward Healing
Avoid DIY pitfalls and recognize infection signs
Ingrown toenails occur when the nail edge penetrates the surrounding skin, causing inflammation and pain. Attempting "bathroom surgery" with non‑sterile tools like nail clippers, tweezers, or needles often damages the nail matrix and introduces bacteria, worsening the condition.
Watch for infection signs: throbbing pain, spreading redness, pus or cloudy drainage, foul odor, and fever. These symptoms demand prompt professional care, especially for patients with diabetes, peripheral neuropathy, or poor circulation.
Seek podiatric care for permanent solutions
Podiatrists treat ingrown nails with a partial nail avulsion under local anesthesia, removing the offending edge and cleaning the wound. For recurrent cases, a matrixectomy — using a chemical or laser — destroys the nail matrix to prevent regrowth. These in‑office procedures provide immediate pain relief and lower recurrence rates below 5%.
Adopt preventive footwear and nail‑care habits
Trimming nails straight across, leaving a small white tip, and avoiding rounded edges are essential. Wear shoes with a wide toe box, rotate footwear to reduce moisture, and keep feet clean and dry. Consistent preventive habits reduce the risk of future ingrown toenails.
