Why Custom Orthotics Matter
Foot biomechanics—how the arches, heel, and toes move during walking—drive the forces transmitted up the kinetic chain. When alignment is off, excess stress can cause plantar fasciitis, heel pain, knee strain, and lower‑back discomfort. Custom orthotics are individually molded to the patient’s exact foot shape, providing targeted arch support, heel stabilization, and cushioning that realign the foot and redistribute pressure evenly. This correction relieves pain at its source and reduces abnormal loading on joints and soft tissues. By restoring a neutral gait, orthotics also prevent secondary injuries such as shin splints, stress fractures, and overuse tendonitis, helping patients stay active and avoid surgical intervention.
Understanding How Orthotics Change Your Gait
 Gait mechanics rely on a coordinated chain of movements that begin at the foot and travel upward through the ankle, knee, hip and spine. When the foot collapses (overpronation) or rolls outward (supination), the kinetic chain is disrupted, increasing stress on joints and soft tissues and often leading to pain in the heel, knee, hip or lower back.
Gait mechanics rely on a coordinated chain of movements that begin at the foot and travel upward through the ankle, knee, hip and spine. When the foot collapses (overpronation) or rolls outward (supination), the kinetic chain is disrupted, increasing stress on joints and soft tissues and often leading to pain in the heel, knee, hip or lower back.
Custom orthotics are fabricated after a detailed gait analysis—using pressure‑mapping, 3‑D scanning or video capture—to identify the exact biomechanical deficits. Functional (semi‑rigid) orthotics control excessive motion, while accommodative (soft) orthotics cushion high‑pressure zones. By providing targeted arch support, heel stabilization and pressure redistribution, the orthotic re‑positions the foot into a more neutral alignment, thereby correcting the underlying biomechanical error.
Clinical studies support these mechanisms. Research on gait‑analysis‑driven orthotics shows measurable reductions in pronation angle, narrower base of support and improved stride symmetry. Patients report up to a 40‑60 % decrease in pain scores and a noticeable shift toward a smoother, more efficient walking pattern within the first month of wear. The combined evidence confirms that properly fitted custom orthotics not only relieve symptoms but actively reshape gait for long‑term functional benefits.
Improving Gait: Benefits of Custom Orthotics
 Custom orthotics are a cornerstone of modern podiatric care for anyone seeking a more efficient and pain‑free gait. By capturing the exact contours of a patient’s foot through plaster casts, foam impressions, or 3‑D scanning, clinicians fabricate inserts that realign the foot, ankle, and lower‑extremity kinetic chain. This alignment reduces excessive pronation or supination, redistributes plantar pressures, and provides targeted arch support that stabilizes the foot during stance and push‑off phases. The result is a smoother stride, less muscle fatigue, and a lower risk of secondary injuries to the knees, hips, and lower back.
Custom orthotics are a cornerstone of modern podiatric care for anyone seeking a more efficient and pain‑free gait. By capturing the exact contours of a patient’s foot through plaster casts, foam impressions, or 3‑D scanning, clinicians fabricate inserts that realign the foot, ankle, and lower‑extremity kinetic chain. This alignment reduces excessive pronation or supination, redistributes plantar pressures, and provides targeted arch support that stabilizes the foot during stance and push‑off phases. The result is a smoother stride, less muscle fatigue, and a lower risk of secondary injuries to the knees, hips, and lower back.
Can orthotics improve gait? Yes—custom orthotics can significantly improve your gait. They correct biomechanical abnormalities, align your feet, ankles, and legs, and redistribute pressure to reduce abnormal motions that cause calluses, stress fractures, and joint pain. This is especially beneficial for individuals with high arches or flat feet, who are more prone to gait‑related issues. By enhancing arch support and tailoring cushioning to specific conditions such as plantar fasciitis, Achilles tendinitis, bunions, or diabetic foot concerns, custom orthotics not only relieve pain but also prevent the progression of deformities and promote better overall posture. Regular follow‑up appointments and proper footwear maximize these benefits over the long term.
Footwear Choices: What to Avoid
 Problematic shoes are any style that fails to support the foot’s natural architecture. Podiatrists commonly advise patients to stay away from high‑heeled shoes, flip‑flops, overly flexible slip‑ons, pointed‑toe boxes, and flat‑sole footwear because these designs promote excessive pronation or supination, compress the arch, and increase stress on the knees, hips, and lower back. Wearing shoes that lack a stable heel, adequate arch support, or a wide toe box can negate the benefits of custom orthotics and accelerate foot pain. The best approach is to choose shoes with firm midsoles, supportive arches, and a roomy toe area, and to pair them with properly fitted orthotics. Regular follow‑up with a podiatrist ensures the footwear remains compatible with evolving foot mechanics.
Problematic shoes are any style that fails to support the foot’s natural architecture. Podiatrists commonly advise patients to stay away from high‑heeled shoes, flip‑flops, overly flexible slip‑ons, pointed‑toe boxes, and flat‑sole footwear because these designs promote excessive pronation or supination, compress the arch, and increase stress on the knees, hips, and lower back. Wearing shoes that lack a stable heel, adequate arch support, or a wide toe box can negate the benefits of custom orthotics and accelerate foot pain. The best approach is to choose shoes with firm midsoles, supportive arches, and a roomy toe area, and to pair them with properly fitted orthotics. Regular follow‑up with a podiatrist ensures the footwear remains compatible with evolving foot mechanics.
Types of Custom Orthotics and Their Roles
 Custom orthotics fall into two functional categories. Functional (or semi‑rigid) orthotics are made from materials such as graphite, carbon fiber, or hard plastics; they realign the foot and control excessive motion, making them ideal for correcting overpronation, supination, and reducing stress on the knees, hips, and lower back. Accommodative (soft) orthotics use cushioned foams, EVA, or silicone to absorb shock and relieve pressure on sensitive areas, benefiting conditions like plantar fasciitis, arthritis, and diabetic foot care. While functional devices are often described as rigid, some semi‑rigid options blend flexibility with support, whereas accommodative inserts are typically softer and more pliable. Material choice—rigid polymers, semi‑rigid composites, or soft foams—depends on the patient’s biomechanical deficit, activity level, and therapeutic goal, ensuring personalized support and optimal gait correction.
Custom orthotics fall into two functional categories. Functional (or semi‑rigid) orthotics are made from materials such as graphite, carbon fiber, or hard plastics; they realign the foot and control excessive motion, making them ideal for correcting overpronation, supination, and reducing stress on the knees, hips, and lower back. Accommodative (soft) orthotics use cushioned foams, EVA, or silicone to absorb shock and relieve pressure on sensitive areas, benefiting conditions like plantar fasciitis, arthritis, and diabetic foot care. While functional devices are often described as rigid, some semi‑rigid options blend flexibility with support, whereas accommodative inserts are typically softer and more pliable. Material choice—rigid polymers, semi‑rigid composites, or soft foams—depends on the patient’s biomechanical deficit, activity level, and therapeutic goal, ensuring personalized support and optimal gait correction.
Integrating Orthotics into a Comprehensive Care Plan
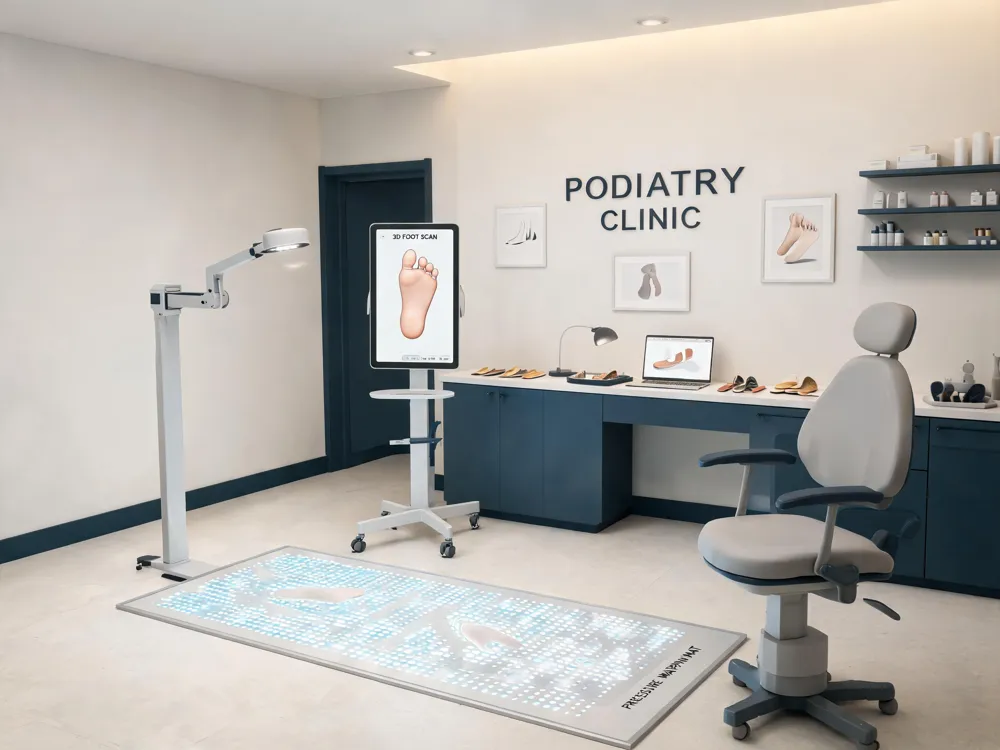 Gait analysis – the foundation of custom orthotic therapy
Modern podiatric clinics begin orthotic prescription with a detailed gait analysis, using pressure‑mapping sensors, motion‑capture cameras, or 3‑D foot scans to identify overpronation, supination, or uneven weight distribution. By pinpointing the exact biomechanical deficits, clinicians can design orthotics that reposition the foot, redistribute forces, and promote a neutral stance‑phase, which research shows reduces plantar pressure peaks by up to 30% and alleviates heel‑pain conditions such as plantar fasciitis.
Gait analysis – the foundation of custom orthotic therapy
Modern podiatric clinics begin orthotic prescription with a detailed gait analysis, using pressure‑mapping sensors, motion‑capture cameras, or 3‑D foot scans to identify overpronation, supination, or uneven weight distribution. By pinpointing the exact biomechanical deficits, clinicians can design orthotics that reposition the foot, redistribute forces, and promote a neutral stance‑phase, which research shows reduces plantar pressure peaks by up to 30% and alleviates heel‑pain conditions such as plantar fasciitis.
Follow‑up care – ensuring lasting effectiveness After the initial fitting, a series of follow‑up appointments is essential. Adjustments fine‑tune arch support, heel wedges, or medial posting to accommodate changes in foot shape, activity level, or weight. Regular visits also verify that footwear properly accommodates the orthotic, a factor that maximizes durability and prevents secondary injuries.
Children and athletes – tailored strategies For growing children, orthotics are replaced when shoe size increases by two sizes to stabilize developing arches and prevent progression of deformities. Athletes benefit from semi‑rigid functional orthotics that control excessive motion while providing shock absorption, reducing the risk of stress fractures, shin splints, and knee pain. In both populations, custom devices outperform over‑the‑counter inserts by delivering individualized support and long‑term biomechanical correction.
Putting It All Together
Custom orthotics provide lasting therapeutic value by continuously correcting foot alignment, redistributing forces, and stabilizing the kinetic chain. Over time, this reduces stress on the plantar fascia, Achilles tendon, knees, hips and lower back, which helps prevent chronic conditions such as plantar fasciitis, arthritis, and tendonitis. The durable, semi‑rigid or soft materials maintain their corrective shape for years, and regular follow‑up appointments ensure the device adapts to weight changes, activity levels, or growth in children.
Preventive care is built into the orthotic workflow. A thorough gait analysis and pressure mapping identify biomechanical deficits before they cause injury. By providing targeted arch support, heel stabilization, and shock absorption, orthotics normalize gait patterns, improve posture, and lower the risk of overuse injuries, stress fractures, and diabetic foot ulcers. Pairing the device with appropriate footwear, routine foot‑care hygiene, and periodic reassessment creates a proactive strategy that keeps patients pain‑free and reduces the need for surgical or other invasive interventions.
